Sheep & Goats

This is an excerpt of Dairy Goat and Sheep Operations in the Southeast Production Guide, ANR-2457.
Estimating the Age of Goats and Sheep
The approximate age of goats and sheep can be determined by their teeth, as illustrated in figure 7. At birth, kids and lambs have eight milk teeth, or temporary incisors, arranged in four pairs on the lower jaw. The central pair of temporary incisor teeth is shed and replaced by the permanent teeth at approximately 1 year of age. At 2 years, a pair of permanent incisors replaces the second pair of milk teeth. At 3 and 4 years, the third and fourth pairs, respectively, of permanent teeth appear. At 4 years of age, the goat or sheep has a full mouth.
The amount of wear on the permanent teeth is an indication of the approximate age of animals older than 5 years. When a ewe or doe loses some of her incisor teeth, she is called a broken mouth.
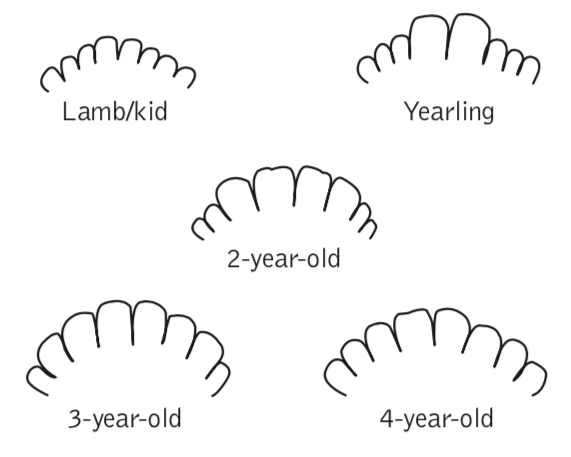
Figure 7. Approximate age of a goat based on its teeth size and shape
Body Condition Scoring
Body condition scoring (BCS) can be a quick and easy method to determine how thin or fat goats/sheep are as individuals and as a herd. Determining BCS can be done in 15 to 20 seconds.
Body condition scoring is based on a numerical scoring system from 1 to 5 with half scores (such as 3.5) given for animals between two scores. A BCS 1 represents an emaciated animal, while a BCS 5 represents an extremely obese animal. It is important to remember that BCS cannot be evaluated by simply looking at the goat/sheep, as hair can hide poor body condition; the evaluator must feel for the amount of muscle and fat cover.
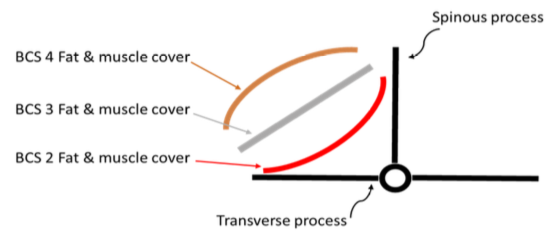
Figure 8. Schematic representation of the vertebrae and muscle:fat covering in a goat:sheep (Adapted from www2.luresext.edu:goats:research:bcshowto.html)
Body condition scoring as part of a routine management program can help the producer effectively monitor feeding and herd health. Low BCS in an individual animal may indicate disease or poor appetite. In a herd of goats/sheep, a large number of animals with low BCS may represent poor overall nutrition or poor management leading to herd health issues.
Body condition scoring is most commonly assessed by evaluating the amount of muscle and fat covering the loin area between the spinous processes and the transverse processes, the sternum, and the ribcage. The evaluator should feel for the amount of tissue covering the ends of the spinous and transverse processes. The amount of fat and loin muscle also should be evaluated. In animals with a low BCS, the bones feel sharp. As the animal increases in body condition, the bone ends feel more rounded and smooth. When evaluating the sternum, scoring is based on the size of the fat pad that can be pinched. The ribs should then be evaluated for the amount of fat cover.
Table 2. Body Condition Score Characteristics
It is recommended that does have a BCS between 2.5 and 3.5 at breeding and a BCS of 3 to 3.5 prior to kidding. Bucks/rams should be maintained at a BCS of 3 to 3.5 prior to the breeding season
| Body Condition Score | Physical Description - Spinous Process | Physical Description - Transverse Process | Physical Description - Loin Eye Muscle | Physical Description - Fat Cover over Loin Eye Muscle |
|---|---|---|---|---|
| 1 | Sharp and prominent | Sharp | Shallow | None |
| 2 | Sharp and prominent | Smooth, slightly rounded | Medium depth | Little |
| 3 | Smooth and rounded | Smooth, well covered | Full | Medium |
| 4 | Easy to feel with pressure | Unable to feel | Full | Thick |
| 5 | Unable to feel | Unable to feel | Very full | Very thick |
Common Management Procedures
Hoof Trimming
Lameness associated with abnormal hoof growth is quite common in goats/sheep. This abnormal hoof growth is most likely due to anatomical abnormalities, environmental influences, and nutritional factors. Hoof overgrowth is commonly a result of increased nutritional intake, especially increased protein in the diet.
Hoof problems also tend to be more of a problem on soft ground or surfaces. Fewer problems are seen in animals that are able to move about on hard, dry surfaces, because they will wear down their hooves naturally. For animals that have been overfed and suffer from chronic laminitis or rapid hoof growth, hoof trimming may be required every 6 to 8 weeks to minimize problems.
Routine hoof trimming can be easily performed with good restraint and the use of shears, nippers, and a hoof knife. Goats/ sheep may be trimmed standing or lying on their side. Some larger farms may have hoof-trimming stanchions available for use. The goal of trimming hooves is to shape the foot to match the angle of the coronary band so that the sole and the coronary band are parallel. The toe, walls, and sole also may be shaped to correct many hoof problems. Proper hoof trimming and management often prevents hoof disorders.
In addition to trimming, a well-balanced diet with a good mineral program prevents hoof disorders. The key is not to overfeed grains, which can lead to rumen acidosis, to maintain a good mineral program, and to ensure an environment that allows for routine wear of the hoof.
Disbudding/Dehorning
Some producers prefer that goats/sheep have their horns removed. Others (mainly meat, fiber, and pet goat owners) prefer to keep horned animals. Disbudding is more commonly performed in dairy goats/sheep to reduce the risk of injuries related to fighting.
Disbudding is best performed during the first 2 weeks of life. This procedure is performed with the kid/lamb restrained and sedated, and the site around the horns clipped and locally anesthetized. A commercial electric dehorning iron or an electric cautery unit can be used to burn the area around the base of the horn until it reaches a copper color. If the cautery iron has been applied correctly, a horn cap should be easily removed. Complications include underheating, which can lead to scur or horn remnant formation, or overheating, which can be very dangerous and lead to heat-induced meningitis or inflammation of the brain.
An alternative to cauterization is surgical disbudding. A veterinarian should perform surgical disbudding when the animal is between 2 and 4 days of age. A caustic paste may also be used to disbud; it is applied to the base of the horn buds after the hair has been clipped. Caution should be used to ensure that the caustic paste does not have contact with other areas of the skin or eyes.
Kids/lambs older than 2 to 3 weeks, goats/sheep with scurs, or adult goats/sheep will all require surgical dehorning. It is recommended that adult animals with large horns undergo general anesthesia before dehorning. Sedation and local anesthetic may also be used. A veterinarian must perform surgical dehorning. In older animals, this may leave an opening into the sinus that requires bandaging for a period of time.
Castration
Castration of a young male is one of the most commonly performed procedures in goats/sheep. There is a growing trend to delay castration in male goats/sheep that are fed a high-concentrate diet (pets, show animals, etc.) to help prevent urolithiasis or urinary blockages.
Castration techniques can be divided into two basic categories: nonsurgical (bloodless) and surgical. Nonsurgical, or bloodless, methods include the use of elastrator bands or the Burdizzo emascu- latome.
The elastrator band should be used in kids/lambs younger than 1 week of age, typically at the time of disbudding/dehorning. Complications include misplacement of the band so that one testicle is above the band.
The Burdizzo emasculatome is used to crush the spermatic cord in two separate locations within the scrotum, which then causes the testicle to atrophy or shrink without damaging the skin of the scrotum. Complications with the emasculatome include inadequate crushing of the cord and maintenance of a functional testicle.
It is important to remember that tetanus can be a major concern in goats/sheep undergoing routine procedures such as castration and dehorning. Producers should ensure that kids/lambs and does/ewes are up to date on tetanus vaccination prior to undergoing routine procedures.
Temperature Reading
A thermometer is an important diagnostic tool to always have on hand. Before contacting a veterinarian about your goat or sheep, it pays to know its temperature. This helps in diagnosing its condition.
Have several working thermometers on your farm at all times. Place them where they are easily accessible to your work area. A good mercury-ring top or digital thermometer can be purchased from most farm supply stores for about $12.00.
The healthy temperature of both goats and sheep is 102.3 degrees F (± 1 degree F). A goat or sheep’s temperature will fluctuate during the course of a day, raising a nominal amount during the heat of the day.
Temperature is measured rectally. Never use a dirty thermometer, even if several animals appear to be suffering from the same problem. A thermometer should be cleaned with an alcohol wipe after each use, secured in its case, and stored at room temperature. Glass thermometers must be shaken down before and after each use. Never run or agitate your animal immediately before taking its temperature; this will lead to a false reading. If your animal appears sick, take its temperature immediately; later in the day or tomorrow is too late.
How to Measure Temperature
For baby goats and sheep, the most comfortable position is to simply lay them across your lap.
For adult or larger animals, it’s helpful to have someone else hold the animal in a standing or reclined position while you take its temperature. For animals that are not very tame, it may be easier to secure them with a collar and rope to a gatepost. Even if you have your animal secured, you may still need someone to help steady it until you insert the thermometer and obtain a reading.
Lubricate the probe end with mineral oil or petroleum jelly and gently insert the thermometer into the rectum. Never force a thermometer; it should slide easily when lubricated. Insert to half the thermometer’s length (about 21⁄2 inches) and hold in place for a minimum of 2 minutes. If your animal’s temperature is high (over 103.5 degrees F), consult your veterinarian to develop a treatment plan.
Common Signs of a Sick Goat or Sheep
Basic Physiological Norms of Goats and Sheep
- Rectal temperature of goats and sheep: 102.3 degrees F (± 1 degree F)
- Heart rate of goats: 70 to 135 beats per minute (90 bpm average)
- Heart rate of sheep: 60 to 120 beats per minute (75 bpm average)
- Respiratory rate of adult goats: 12 to 20 breaths per minute
- Respiratory rate of adult sheep: 19 breaths per minute
Listed below are some of the most common signs of a sick goat/ sheep. Observe your animals daily and know their normal behavior. Remember, these animals are herd/flock oriented; if separated, they will exhibit some of the same signs as well.
Goats/sheep who isolate themselves from the herd/flock. The most common initial signs of a sick goat or sheep are one that is not eating or drinking and is standing with its head and tail down away from others.
Teeth grinding or gritting. This is a sign of pain and an early sign of a sick animal.
Weight loss in normally well-conditioned goats/sheep. Older animals are much thinner than younger ones; you must know who is older and who should be well muscled.
Scourers (diarrhea). Observed on the rear of goat or sheep, this is the result of parasite infestation, coccidia, pneumonia, or a variety of other diseases.
Cloudy, runny, or closed eyes. This is a possible indication of pinkeye or parasites. A severely infected animal will have a purulent (an infected watery liquid) discharge from its eyes, and the tissue under the eyelid will be extremely pale pink. (This tissue is normally a bright pink.)
Stargazing. A goat or sheep that holds its head up as if looking at the stars could be exhibiting a sign of listeriosis or polio.
Drunken gait. A goat/sheep that staggers as it walks could exhibit another sign of polio.
Stiff sawhorse appearance. This could be a sign of tetanus. Look for puncture wounds over the animal’s entire body. Kids/lambs who have been disbudded or castrated recently will demonstrate this appearance. It is always a good idea to prevent this with an injection of tetanus antitoxin at the time of disbudding or castration; this provides an additional 7 to 10 days of protection.
Dull, scruffy coat. This is a potential sign of intestinal worms, lice, or copper deficiency.
Runny nose. This is a possible indication of pneumonia.
Oliguria (decreased urine output). This is a potential symptom of urinary calculi in bucks and wethers and a sign of urinary infection in does/ewes.
Constipation/not defecating. This is indicative of digestive upset.
Scrapie Disease
Scrapie is a degenerative and fatal disease that affects the central nervous system of goats and sheep. It is classified as a transmissible spongiform encephalopathy (TSE). The means of transmission is not completely understood, but animals are most likely infected as kids/ lambs. Once an animal is infected, the animal remains infected for life.
Initial signs of scrapie present 2 to 5 years after infection. Most animals do not show signs of the disease until they are at least 2 years of age. The average age of clinical onset of disease is 3 to 4 years.
In the beginning, clinical signs may be subtle or noticed only occasionally. Animals first exhibit behavioral changes, such as aggression, a fixed gaze or stare, or failure to respond to human interactions. These affected animals will begin rubbing and biting their tail head, rump, thighs, and back. The pruritis (itching) becomes more persistent and often leads to self-inflicted trauma.
As the disease progresses, goats/sheep may have difficulty milking, premature kidding, and pica (eating or licking an unusual substance). Infected animals will also become ataxic, or uncoordinated in their movements, and will begin to lose weight.
Affected animals eventually separate from the herd and go off feed. The animal eventually is unable to stand and may develop convulsions. There is no effective treatment for scrapie available. Early diagnosis and removal of affected animals from the herd/flock are critical to prevent transmission.
Eradication of the disease from the herd/flock may consist of selective depopulation of high-risk exposed animals—animals that have been heavily exposed, test positive/inconclusive, or show clinical signs. Less commonly, complete herd depopulation may be recommended. All goats and sheep are considered to be genetically susceptible to scrapie.
Scrapie is a reportable disease. If signs or concerns of disease in goats/sheep older than 12 months of age arise, contact the state veterinarian or the USDA Veterinary Services area office. Diagnostics can be made in either live or deceased animals.
As of 2001, the United States Department of Agriculture’s Animal and Plant Health Inspection Service requires all goat and sheep producers to observe established federal and state regulations of official identification methods of their animals. In the state of Alabama, goats and sheep must be registered and identified by an ear tag or tattoo prior to any sale or transport.
For more information on the National Scrapie Eradication Program or to order scrapie tags, phone (866) 873-2824.
Diseases to Vaccinate Against
Vaccines are available for many diseases. But not all diseases are a routine threat to many goat and sheep dairies, and some vaccines are not sufficiently effective to justify their use. Therefore, every farm will have unique vaccination requirements based on individual goals.
The following guidelines for vaccinating goats and sheep may not be applicable in all situations. The best use of these guidelines is as a starting point to develop an effective vaccination protocol with your veterinarian or Extension agent. As applicable, ensure that products are safe for pregnant animals and for kids/lambs nursing pregnant does/ewes.
Properly store and administer vaccines according to label directions or veterinary prescriptions, and adhere to designated milk and meat withdrawal times. If there is a discrepancy between these guidelines and product label directions, defer to the product label.
Campylobacteriosis (vibriosis). Vaccinate ewes against vibriosis 30 days before breeding and repeat 60 to 90 days later. An annual booster is required.
Caseous lymphadenitis (CL). Commercial vaccines are available for goats and sheep against caseous lymphadenitis (CL). Administering clostridium CD/T plus a CL vaccine can produce a strong adverse reaction and is not recommended.
Chlamydia. A killed vaccine to prevent chlamydial abortion in sheep is available. Vaccinate ewes 60 days prior to breeding, and booster 30 days after the first dosage. This vaccine is not labeled
for use in goats; however, it seems to be somewhat effective and might be prescribed by your veterinarian for such use. The vaccine produces side effects that include muscular soreness and stiffness, and the vaccine can cause abortion if goats are vaccinated during the first 28 to 45 days of pregnancy.
Clostridial diseases. Vaccinate pregnant does and ewes against clostridial diseases during the fourth month of pregnancy. This vaccine is commonly referred to as the clostridial CD/T vaccine. Herd bucks and rams may also receive annual CD/T vaccinations at this time. Vaccinate kids and lambs against enterotoxemia and tetanus at 3 months of age. A booster should be administered according to FDA-approved label directions, usually 3 to 4 weeks following the initial dose and once annually thereafter.
Foot rot. In sheep flocks, vaccinate 2 to 4 weeks prior to the rainy season, with a booster between 6 weeks and 6 months later. Boosters should be given twice a year, 1 to 2 weeks prior to expected outbreaks. The vaccine causes a localized raised lump at the injection site and is not recommended for use in pregnant ewes. The FDA has not approved this vaccine usage in goats.
Leptospirosis. Vaccinate against leptospirosis in regions where the disease is prevalent, or in case of an outbreak under a veterinarian’s guidance.
Pneumonia. Vaccinate pregnant does and ewes during the fourth month of pregnancy against pneumonia caused by Pasteurella multocida or Mannheimia haemolytica. Kids and lambs vaccinated when less than 3 months of age should be revaccinated at weaning or at 4 to 6 months of age.
Rabies. There are several killed virus rabies vaccines made for sheep that are not labeled for goats. The vaccines seem to be effective in goats, however, and may be prescribed by your veterinarian. Vaccination against rabies is especially recommended in case of an outbreak in your area.
Vaccination Guidelines
Vaccinations are a precaution that goat and sheep producers should adopt into their herd health plan to help prevent introduction and spread of infectious diseases. Consult your local veterinarian and Extension agent for diseases commonly vaccinated against in your area.
Three types of vaccines are available for sheep and goats:
- Modified-live vaccines use live microorganisms that replicate in the animal after injection. This has been termed a controlled infection, since the organisms have been modified so that they do not cause disease but still stimulate the immune system. This type of vaccine often causes a quick and prolonged response of the animal’s immune system. The vaccine for sore mouth disease is an example of a modified-live vaccine.
- Killed vaccines use killed (inactivated) bacteria or virus and adjuvant. The adjuvant helps create a stronger immune response in the animal’s body. Most pneumonia vaccines are killed vaccines.
- Toxoid vaccines provide immunity against bacteria that produce disease-causing toxins. Toxoid vaccines, such as those for enterotoxemia and tetanus, use bacterial toxins that have been rendered harmless to stimulate immunity against the toxin.
General Vaccination Guidelines
- Follow all FDA-approved manufacturer’s guidelines for vaccine dosage, storage, route of administration, boosters, and expiration date.
- Avoid drug residues in meat and milk by following the FDA-recommended withdrawal times printed on the product label for treated animals that will enter the food chain via slaughter or will provide milk for human consumption.
- Use sterile needles and use a new needle for each animal.
- Administer vaccines to adult goats and sheep using a 20-gauge 1-inch needle.
- Use 1/2-inch needles for smaller does/ewes and kids/lambs.
- Keep used needles in a safe, rigid container for disposal. • Keep vaccination records.
- Consult a veterinarian for disease control and product information.
Booster Vaccinations
A second (booster) vaccination may be required for young animals being vaccinated for the first time. A booster vaccination is definitely required for killed vaccines to provide optimal protection. FDA-approved product label directions indicate when and if a booster vaccination is required. Consult your veterinarian if there are any questions about if and when booster vaccinations should be administered. Failure to give the booster at the proper time could result in an incompletely protected adult animal, even if it is vaccinated every year thereafter.
Proper Handling of Vaccines
The best vaccine program will fail if the product is damaged by improper handling. For example, if the label says to store a vaccine at 35 to 45 degrees F, the vaccine should be refrigerated. Vaccines should not be allowed to freeze, nor should they be stored in direct sunlight.
Most modified live vaccines must be reconstituted by adding sterile water to a dehydrated cake in a separate sterile vial. Once the water is added, the vaccine organisms are fragile and will be live for only a short time. As a rule, only reconstitute enough vaccine to be used within 30 to 45 minutes. Use a cooler or other climate-controlled storage container to protect reconstituted vaccines from extremes of cold, heat, and sunlight.
Do not mix different vaccines together in one syringe or combine other injectable drugs into the same syringe with vaccines. Although this method has been advocated as a method of reducing the number of injections, it will inactivate vaccines because of incompatibilities with the other compounds.
Treatment and Drug Handling
Even with superior herd/flock management, some animals will become sick or injured. The decision to treat sick or injured animals should be based on specific criteria:
- Will the animal return to a healthy, productive state without treatment?
- Will treatment return the animal to a healthy, productive state?
- What treatment best fits the herd and disease management?
- Should the animal be sold?
- Should the animal be euthanized?
Storing, Handling, and Using Drugs Correctly
Drug performance declines if the expiration date has passed, if the storage temperature is too hot or cold, or if the drugs have been improperly exposed to air or light. All the information you need to properly store, handle, and administer any animal health product should be available on FDA-approved drug labels or on a veterinarian’s prescription. Following are general guidelines:
- Check the expiration date on the label.
- Do not save partially used bottles of vaccines. They will not be effective for later use and may be contaminated.
- Some drugs, and most vaccines, need to be refrigerated but not frozen. Keep an accurate thermometer in your refrigerator to monitor the temperature.
- Use disposable syringes. Use clean needles to draw contents from multi-dose bottles. Change needles at least every 10 to 15 animals to minimize disease spread and drug contamination. Do not store medication in syringes, as they cannot be labeled easily.
- Avoid exposing vaccines and other medicines to direct sunlight. This may degrade the product. Use an insulated cooler for storing syringes and drugs while working on animals to avoid sunlight and maintain the proper temperature.
- Collect used needles in a rigid plastic container. Dispose of them by returning them to your veterinarian. Destroy disposable syringes so they cannot be reused or misused.
- Read FDA-approved product labels and veterinary prescriptions. Some drugs and vaccine containers require incineration before disposal. Used needles, scalpels, etc., are considered medical waste and must be handled and disposed of in accordance with the laws that govern them.
- Consult your local veterinarian regarding any questions on proper use of medications.
Biosecurity
A biosecurity plan is an innovative approach to managing the risk of disease introduction and spread on your farm. It is designed to help livestock producers identify disease risks and manage them through practical measures for common, everyday infectious diseases, as well as new or unexpected diseases. An effective biosecurity plan manages disease by evaluating and addressing the primary routes of disease transmission, therefore controlling several diseases at one time.
There are five primary routes of disease transmission:
- Aerosol transmission occurs when disease agents contained in droplets pass through the air from one animal to another. Close proximity of infected and susceptible animals is typically required for aerosol transmission.
- Direct contact transmission occurs when a susceptible animal directly touches an infected animal through its open wounds, mucous membranes, blood, saliva, nose-to-nose contact, rubbing, or biting.
- Fomite transmission occurs when a disease pathogen is carried or spread from one animal to another by an inanimate object (such as boots, buckets, and milking and grooming equipment). Vehicles, trailers, and even humans can be considered fomites and can spread disease through traffic transmission.
- Oral transmission occurs when an animal licks or chews on contaminated environmental objects or consumes contaminated feed or water.
- Vector-borne transmission involves the spread of disease through an insect. Ticks and mosquitoes are biological vectors, commonly spreading disease after becoming infected from a diseased animal and injecting the disease agent into another animal. Flies are common mechanical vectors of disease, as they carry the disease agent on their bodies and pass it from one animal to another.
A biosecurity plan involves multiple components but results in practical measures for implementation. The first step is assessing the risk areas on a livestock facility based on the possible routes of disease transmission. After identifying risk areas, prioritize disease management measures and implement them. The following are examples of biosecurity practices that will greatly minimize the risk of disease introduction and transmission:
- Do not intentionally commingle animals from different herds.
- Provide a buffer between adjoining herds so that no fence-line contact is available.
- Isolate new herd additions for 4 to 6 weeks and have your veterinarian test for appropriate diseases before allowing new animals to commingle with your herd. Identify isolation areas prior to purchase.
- Isolate animals returning from livestock shows.
- Post signs indicating that a biosecurity plan is in effect on your farm.
- Educate all visitors about the biosecurity plan in effect on your farm.
- Ensure that all visitors are dressed appropriately. Provide coveralls and boots, or make sure visitors are wearing clothing free from contact with other livestock.
- Recognize that you are also a source of contamination for your herd. If you are around other livestock, shower and change clothes before working with your animals.
- Clean and disinfect your truck and trailer after hauling livestock. Anyone hauling livestock for you should do the same.
- Clean and disinfect other equipment as necessary.
- Apply appropriate insect control.

